Pilot
Diabetic retinopathy
México. Jalisco
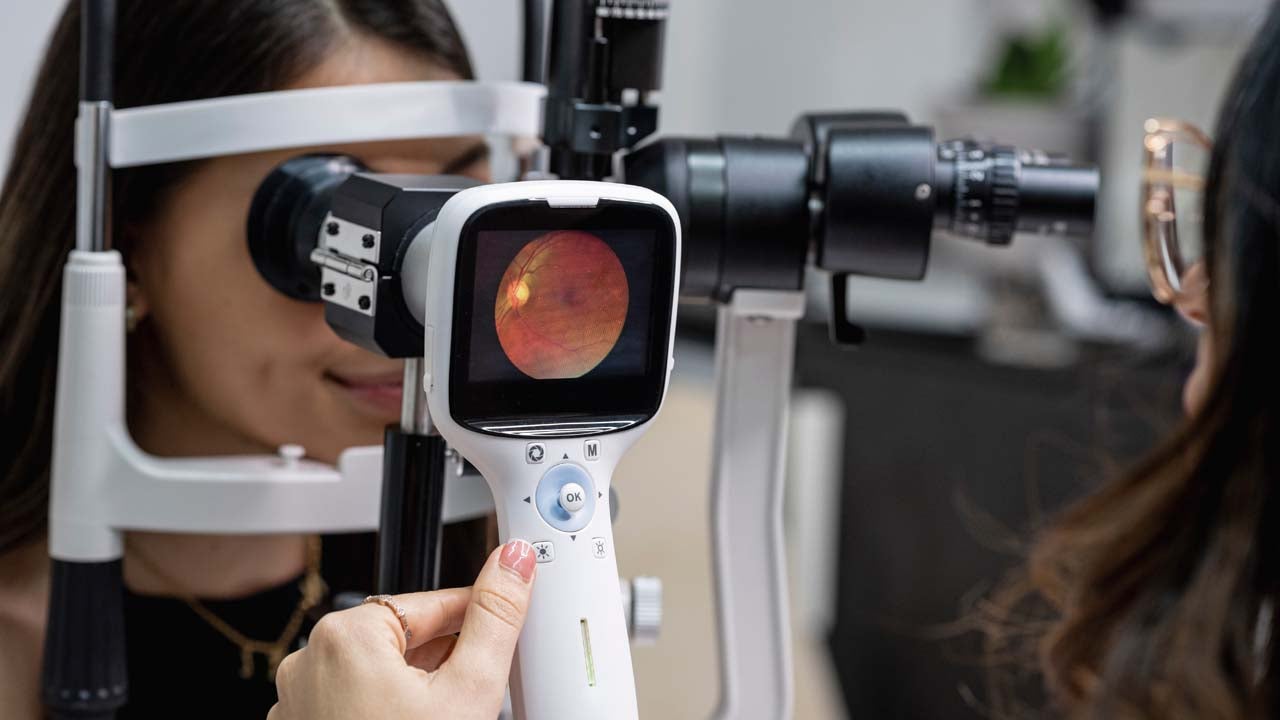
Diabetes mellitus (DM) is one of the most common chronic diseases in most countries. In Mexico, it is estimated that by 2030, 16.4 million people will be affected by this disease. Diabetic retinopathy (DR) is an eye condition derived from DM, caused by high blood sugar levels, which can lead to vision loss and even blindness. Data reported by the National Health and Nutrition Survey (Encuesta Nacional de Salud y Nutrición, ENSANUT) show that impaired vision is the complication most commonly reported by diabetics in Mexico evidencing the importance of addressing this condition to reduce blindness caused by DR.
Problem to be solved:
This chronic and progressive disease has a prevalence of 31.5 percent in Mexico, and in industrialized countries it has become the main cause of partial visual loss and blindness in adults. In the absence of symptoms at the beginning of the disease, an ophthalmological examination is important at least every six months. Early detection facilitates treatment to reduce vision loss and hence blindness.
Populations that are affected by the problem
People with Diabetes Mellitus of working age
Current response to this problem, considering related institutions.
Currently both the official Mexican standard NOM-015-SSA2-2010, focused on the prevention, treatment and control of diabetes mellitus, as well as the clinical practice guidelines, indicate that the detection of the pathology is carried out by examination of the fundus under pupillary dilation by an ophthalmologist following two main schemes:
Type 1 Diabetics
For people diagnosed with type 1 diabetes before puberty, screening for
Diabetic retinopathy should be started at puberty with annual follow-up, unless there are
other considerations that suggest the need for a prior examination.
For people with type 1 diabetes diagnosed after puberty, screening for
Diabetic retinopathy should begin 3-5 years after the diagnosis of diabetes and
thereafter, every year or earlier than needed.
Type 2 Diabetics
People with diabetes and good metabolic control who do not have retinopathy lesions
diabetic at the initial examination (at the time of diagnosis), should have a fundus examination under drug mydriasis at least every two years. In known patients with diabetes mellitus with initial revision (at the time of diagnosis) without diabetic retinopathy and who have poor metabolic control, they should be evaluated once every year.
Diabetic Pregnant
Patients with type 1 or type 2 diabetes who are considering becoming pregnant should be
advised to undergo an ophthalmological evaluation before trying to conceive. Further,
Assessments should be conducted during the first trimester and as indicated by the stage of the
retinopathy and the rate of progression during the rest of the pregnancy and during the first postpartum year.
The literature agrees that those diabetic patients who wish to become pregnant should
The first fundus evaluation should be performed as part of the pregnancy initiation protocol and the follow-up will be as follows according to the result of that initial evaluation:
Without retinopathy, evaluation at 28 weeks
With mild to moderate retinopathy, evaluation between week 16 and 20
With severe or proliferative retinopathy evaluation at 12 weeks
In patients with retinopathy diagnosed during pregnancy should have an evaluation of
fundus 6 months after the baby is born.
DIAGNOSIS People who are diagnosed with diabetes should undergo their first
retinal examination when confirming to be carriers of diabetes mellitus.
As can be seen in the “must be” there is an indication to carry out the screening, however,
Diabetic Retinopathy prevails as one of the main causes of blindness in adults,
which denotes failures in early detection and, therefore, in the process.
At this time the detection is carried out in the first level units, where if they detect any
abnormality or the diabetic patient reports vision problems, they are immediately referred to a
second or third level of care for assessment, in the first level of care is really
little that doctors can do to detect it early.
Although normatively the indication exists, it requires greater monitoring and methods of
more feasible screening, according to reality and available infrastructure.
Proposal to solve this problem using AI:
A DR screening program is required at the first level of health, where patients will be able to come for a visual examination and a computer system will transfer their fundus photographs to the Diabetic Retinopathy Graduation Department. This department is assisted by certified graders and an AI system, which help determine the patient's DR level in order to transfer those cases with an advanced DR level to a second-level hospital for early diagnosis and timely treatment.
What security considerations, national laws or standards have to be taken into account to use each source of information?
For clinical considerations, the official Mexican standard NOM-015-SSA2-2010 and the national DR clinical practice guidelines.
Main AI challenges identified:
Poor quality screening program, absence of protocols and processes in the program considering AI, data governance, staff and patient awareness.
Hub
Sector
Health
Location
Jalisco , México
Executing Entity
Jalisco Government - Tec de Monterrey
State
Contact
It may interest you
En este documento se abordan los impactos de la inteligencia artificial en la educación
En conjunto con la OECD publicamos el manual de ciencia de datos, el cual busca proveer recomendaciones técnicas a los equipos desarrolladores de sistemas de IA.



